Frequently Asked Questions
Understanding the Condition
Microtia is a congenital condition in which the external ear is underdeveloped or absent at birth. Despite the external appearance, the inner ear and hearing nerve are almost always completely normal. This is why both reconstruction and hearing intervention produce reliable, favorable outcomes.
Did I cause my child’s microtia?
No — and this is one of the most important things for parents to understand and to hear clearly. Microtia is not caused by anything you did or did not do during pregnancy. It is not caused by stress, diet, activity, or anything within a parent’s control. Microtia occurs during a very specific and brief window of fetal development — between gestational weeks 4 and 8 — before most women even know they are pregnant, and before most prenatal decisions are made. The biological events that shape the ear are not under parental control. This is not your fault.
Dr. Bonilla has met with families from across the United States and more than 50 countries and this question is asked in nearly every first consultation. The answer is always the same.
— Dr. Arturo Bonilla
What is microtia?
Microtia is a congenital condition in which the external ear is underdeveloped or absent at birth. The word comes from the Latin micro meaning small and otia meaning ear. Microtia occurs in approximately 1 in 6,000 to 12,000 births and ranges in severity from a slightly small but recognizable ear all the way to complete absence of the external ear. Microtia most commonly affects one ear — called unilateral microtia — though both ears can be affected in bilateral microtia. Despite the external appearance, the inner ear and hearing nerve are almost always completely normal.
What causes microtia?
The exact cause of microtia is not fully understood. The most widely accepted theory is that a disruption in blood supply to the developing ear — possibly compression of a small artery — occurs during the first trimester of pregnancy when the outer and middle ear are forming. Interestingly, the vast majority of microtia patients worldwide present with a very similar malformation — Grade III — suggesting a common developmental mechanism. Certain medications taken during pregnancy have been associated with microtia, though these are rare. In most cases there is no identifiable cause.
Can microtia be passed on genetically?
In most cases microtia is not genetically inherited and occurs without any family history. However, genetic causes of microtia are an active area of research. Certain syndromes associated with microtia — such as Treacher Collins syndrome — do have a hereditary component with a meaningful chance of passing to a child. For isolated microtia without an associated syndrome, the recurrence risk in future pregnancies is low — families who are concerned about recurrence are encouraged to consult with a genetics specialist. A consultation with a medical geneticist — part of Dr. Bonilla’s care team — can provide personalized guidance.
Is microtia associated with other conditions?
Microtia can occur as an isolated finding or it can be associated with syndromes affecting other structures of the face and head. The most common associated syndrome is hemifacial microsomia which involves underdevelopment of one side of the face. Treacher Collins syndrome, Goldenhar syndrome, and other craniofacial conditions can include microtia as one component. The overwhelming majority of children with isolated, unilateral microtia have no associated conditions. Dr. Bonilla’s care team includes a medical geneticist who evaluates each patient for associated findings.
How common is microtia?
Microtia occurs in approximately 1 in 6,000 to 12,000 live births worldwide making it a rare but not extremely rare condition. It affects boys slightly more often than girls and the right ear is affected more commonly than the left in unilateral cases. Bilateral microtia affects both ears and occurs in approximately 10% of microtia cases. Dr. Bonilla has treated patients from more than 50 countries representing thousands of families across every continent.
The Four Grades of Microtia — Explained
Microtia is classified into four grades based on severity. Understanding your child’s grade is the foundation for understanding the reconstruction plan, surgical timing, and hearing strategy.
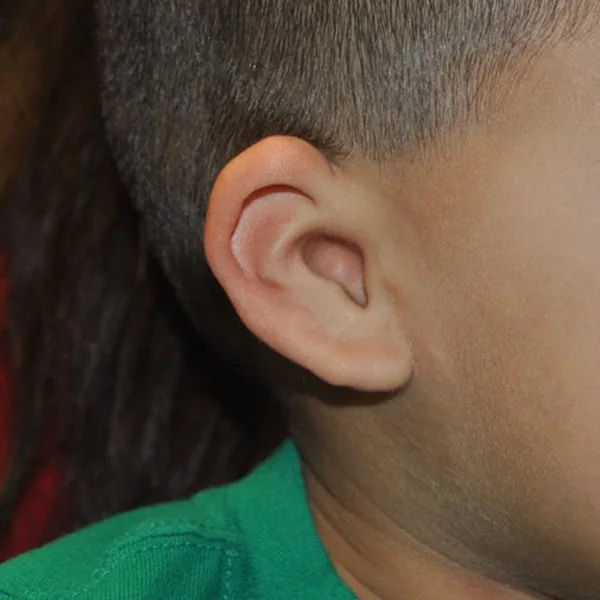
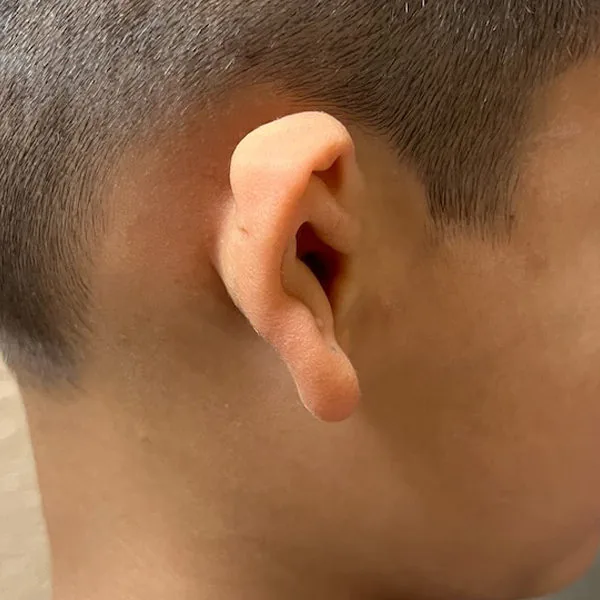
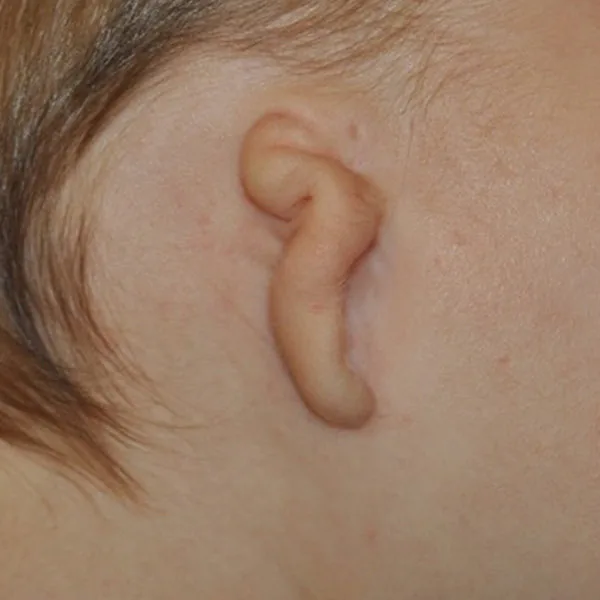
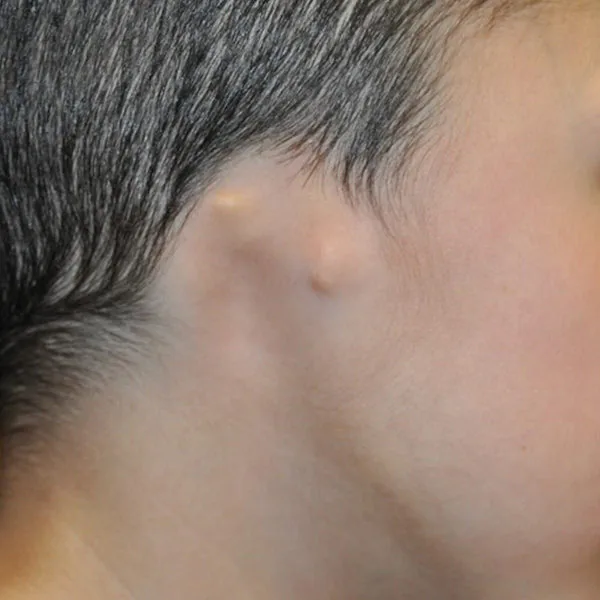
What are the four grades of microtia?
Microtia is classified into four grades based on severity. Grade I is the mildest form — the ear is smaller than normal but all major structures are recognizable and present. Grade II involves partial development — the lower half including the earlobe is typically present but the upper half is absent. Grade III is the most common type — the classic peanut-shaped cartilage remnant with no recognizable ear structures. Grade IV is the most severe — complete absence of the external ear, also called anotia.
Which grade is most common?
Grade III microtia is by far the most common type, accounting for the vast majority of microtia cases worldwide. This is why Dr. Bonilla’s reconstruction technique is built around Grade III anatomy, and why the outcomes across thousands of cases are well-documented.
Does the grade affect hearing?
Yes — grade affects the likelihood and severity of hearing loss. In Grade III and IV microtia the ear canal is almost always absent, causing moderate to severe conductive hearing loss. In Grade II the canal may be present but narrow. In Grade I a functional canal is often present. Crucially, the inner ear — the cochlea and hearing nerve — is almost always completely normal in all grades. The hearing organ works perfectly. It simply cannot receive sound through the absent ear canal.
The hearing organ is almost always completely normal
The cochlea — the inner ear hearing organ — develops from a completely separate embryological structure and is almost never affected by the same disruption that creates microtia. The hearing organ works perfectly. It simply cannot receive sound through the absent ear canal. This is why hearing intervention is so effective and why outcomes are so consistently excellent.
Understanding hearing in microtia patients
Can you still hear if you have microtia?
Yes — but hearing is affected in most cases. The vast majority of patients with microtia and aural atresia have moderate to severe conductive hearing loss. Because there is no ear canal, sound cannot travel through the outer and middle ear to reach the inner ear. The critical good news is that the inner ear and hearing nerve are almost always completely normal. The hearing organ works perfectly — it simply cannot receive sound through the absent ear canal.
What is aural atresia?
Aural atresia is the medical term for absence of the ear canal. It occurs in the majority of microtia cases — particularly Grade III and IV. In aural atresia the ear canal is replaced by a solid plate of bone. This is the primary cause of hearing loss in microtia patients. The inner ear develops from a completely separate embryonic structure and is therefore almost always unaffected.
How is hearing loss treated in microtia patients?
There are several effective options. Bone conduction hearing devices — including BAHA softbands for infants and surgically implanted devices for older children — bypass the absent ear canal and deliver sound directly to the normal cochlea through the skull. Atresiaplasty — ear canal surgery — is an option for carefully selected patients with favorable CT scan findings. Dr. Bonilla coordinates both outer ear reconstruction and hearing rehabilitation as part of a comprehensive treatment plan.
When should hearing intervention begin?
As early as possible — ideally in the first weeks of life. A BAHA softband can be fitted for infants from birth requiring no surgery. Early hearing support is critical for speech and language development and has been shown to dramatically improve language outcomes in children with microtia. Do not wait for reconstruction to begin hearing support.
Surgery Timing & Candidacy
When is the right age for microtia ear reconstruction?
The optimal age is between 6 and 9 years old. By age 6 the rib cage has grown sufficiently to provide enough cartilage for a full-sized ear framework and the opposite ear has reached approximately 85 to 90% of its adult size — allowing Dr. Bonilla to create a closely matched result. Surgery before age 6 risks using cartilage that is too soft and insufficient in volume.
Can microtia reconstruction be done in adults?
Yes — reconstruction can be performed at any age. Adults who did not have reconstruction as children are excellent candidates. Dr. Bonilla has performed successful reconstructions in patients ranging from age 6 through adulthood with no upper age limit for candidacy. Adult rib cartilage is typically more firm which can actually produce excellent structural detail in the framework.
What determines candidacy for surgery?
The primary factors are age of at least 6 years, sufficient rib cartilage development, and overall health. For hearing surgery, a CT scan of the temporal bone evaluates middle ear structures and determines atresiaplasty candidacy. A consultation with Dr. Bonilla provides a personalized candidacy assessment for each child — including age, rib cartilage development, grade, and overall health.
Surgical Outcomes — Key Numbers
Dr. Bonilla has specialized exclusively in pediatric microtia since 1996, performing no other surgical procedure. This degree of exclusive focus is unusual in reconstructive surgery and is reflected in his case volume and published outcomes.
The Surgical Stages
What is distinctive about Dr. Bonilla’s approach to microtia reconstruction?
Dr. Bonilla has devoted his entire surgical career to pediatric microtia — no other procedures, no other patient population. That singular focus is reflected in the depth of his clinical experience.
How many surgeries will my child need?
All stages are spaced approximately 2 months apart. Full reconstruction is complete well within a single year for all grades. For bilateral microtia, Dr. Bonilla’s coordinated staging approach completes both ears in approximately 2–6 months.
What happens during each stage?
Stage 1 — Dr. Bonilla harvests rib cartilage through a small 1 to 1.25 inch incision and sculpts it into a precise six-structure ear framework placed under the skin. This is the primary reconstruction surgery requiring an overnight hospital stay. All subsequent surgeries are outpatient.
Stage 2 — Earlobe rotation, tragus formation, and conchal deepening refine the ear structure. An outpatient procedure with straightforward recovery.
Stage 3 — Elevation lifts the reconstructed ear away from the head giving it natural three-dimensional projection away from the scalp — the final transformation into a fully natural-appearing ear. Stage 3 is outpatient with same-day discharge. A small sponge placed behind the ear is removed at a follow-up visit 5–7 days later.
Does microtia surgery hurt?
Microtia surgery is remarkably well tolerated. Average pain is 1 to 2 on a 10-point scale. An intraoperative epidural placed by the pediatric anesthesiologist provides excellent pain control through the first 24 hours. Most patients need only children’s Tylenol afterward. Parents are consistently surprised by how comfortable their child is.
Results & Longevity
How natural does the reconstructed ear look?
In experienced hands, natural rib cartilage reconstruction produces results remarkably close to a natural ear. Dr. Bonilla uses the mirror image of the normal opposite ear as his template — matching every contour, curve, and structural detail. Results continue to improve as swelling resolves and skin molds to the framework over the first year after each stage.
How long do results last?
Results are long-lasting. Natural cartilage is durable and grows with the child — with good post-operative care, results are expected to last a lifetime. Some loss of definition can occur over time without proper care. Patients reconstructed by Dr. Bonilla decades ago continue to have excellent results today. His earliest patients — children operated on in the late 1990s — are now adults in their thirties with intact, proportionate reconstructions.
Rib Cartilage — The Most Widely Used Reconstruction Technique
Why is rib cartilage the most recommended technique worldwide?
Over the past 50 years, natural rib cartilage has been and remains the gold standard for ear reconstruction worldwide. Approximately 91.3%¹ of microtia surgeons prefer rib cartilage over synthetic implants. Natural cartilage is the patient’s own living tissue — it grows with the child, flexes like a real ear, lasts a lifetime, and carries none of the permanent risks associated with synthetic materials.
Is rib cartilage microtia reconstruction a 3D ear reconstruction?
Yes. Every ear is three-dimensional — a flat ear would not exist. Dr. Bonilla’s technique creates a 3D ear framework hand-sculpted from the child’s own rib cartilage during surgery, shaped to match the child’s contralateral ear and specific anatomy. Medpor and Su-Por reconstruction also produces a 3D ear, but the framework is a pre-formed polyethylene implant manufactured in advance and selected by size. Both approaches result in a three-dimensional ear; they differ in whether the 3D shape is sculpted from the child’s own living tissue or built around a synthetic framework.
Is rib cartilage reconstruction more invasive than Medpor or SuPor?
This is one of the most common misconceptions in microtia care. Synthetic implant surgery typically takes 7 to 10+ hours in a single session. Dr. Bonilla’s rib cartilage reconstruction for Grade II microtia averages approximately 3 hours. For Grade III, each individual stage is shorter than a single synthetic implant surgery. Recovery time is comparable. The critical difference is not invasiveness — it is the material and its lifelong implications.
Single-Stage Rib Cartilage vs. Synthetic Implant — The Facts
| Dr. Bonilla — Natural Rib Cartilage | Medpor / SuPor Synthetic | |
|---|---|---|
| Surgery Time | ~3 hours | 7–10+ hours |
| Material | Patient’s own natural tissue | Synthetic implant (polyethylene) |
| Grows With Child | Yes — living tissue grows | No — plastic never grows |
| Natural Flexibility | Yes — flexes like a real ear | No — rigid for life |
| Lifetime Fracture Risk | None | Yes — permanent risk |
| Exposure Risk | None | Yes — permanent risk |
| Revision If Needed | Moderate difficulty | May need replacement with a slightly smaller implant |
| Sleeping Comfort | Normal | Firm implant material — discomfort when sleeping on the ear commonly reported |
| Preferred By Surgeons | ~91.3%¹ worldwide | Less than 2% |
| Permanent Result | Yes — with good post-operative care | Lifetime exposure and revision risk present |
What are the risks of synthetic implants?
Synthetic implants carry permanent lifelong risks. The most serious are implant fracture and exposure — where the rigid plastic pushes through the overlying skin. These complications can occur at any point in life and are extremely difficult to repair. The synthetic ear does not grow with the child and cannot flex naturally. Revision surgery on a failed synthetic implant is among the most technically challenging procedures in reconstructive surgery.
Will the reconstructed ear grow with my child?
Yes — when natural rib cartilage is used, the reconstructed ear grows with the child because it is living tissue. A synthetic implant does not grow — it remains fixed plastic while the child and the opposite ear continue to grow throughout childhood and adolescence, creating an increasingly visible asymmetry over time.
Bilateral Microtia
Bilateral microtia has unique implications for both reconstruction and hearing because both ears require surgery and hearing loss affects both sides simultaneously.
- More likely to have a genetic or syndromic cause — genetics evaluation is important
- Hearing intervention is urgent from birth — a bilateral BAHA softband within weeks
- Normal language development is achievable with prompt, bilateral hearing support
- Higher recurrence risk in families than unilateral cases
- Both ears reconstructed — typically one at a time
- Two to four stages completed in approximately 5 to 6 months total
- Without a normal opposite ear as template, Dr. Bonilla uses standardized anatomical proportions
- Excellent symmetry achievable with experienced technique
What is bilateral microtia?
Bilateral microtia means both ears are affected, occurring in approximately 10% of microtia cases. It has unique implications for both reconstruction and hearing because both ears require surgery and hearing loss affects both sides simultaneously. Bilateral cases are more likely to have a genetic or syndromic cause, making genetics evaluation important.
How is bilateral reconstruction different?
Dr. Bonilla reconstructs both ears — typically one at a time — with the full bilateral reconstruction completed in approximately 5 to 6 months. Without a normal opposite ear as template, Dr. Bonilla uses standardized anatomical proportions and decades of experience to design both ears for natural symmetry. The surgical technique itself is the same — rib cartilage harvested and sculpted into a precise framework.
How is hearing managed in bilateral microtia?
Hearing intervention is especially urgent in bilateral cases. A bilateral BAHA softband should be fitted as early as possible — ideally in the first weeks of life — to provide hearing input to both sides simultaneously. This bilateral hearing support is critical for normal speech and language development. Without it, language acquisition is significantly impacted. With it, outcomes are consistently excellent.
What families ask most in the first days after diagnosis
Related Resources
The most useful next resources depending on where you are in your journey.
Contact Dr. Bonilla’s Office
Dr. Bonilla and his team are available to answer questions specific to your child — by contact form or phone.
